For many New Yorkers, summer means escaping the heat of the city and
Adventuring outdoors along the Hudson Valley
Relaxing by the pool in the Hamptons
Cooling off in Fire Island
Yet, New Yorkers beware! These locations harbor a pesky insect: the tick.
As if it weren't bad enough that these mini-vampires love the taste of your blood, these critters can transmit bacterial infections, too.
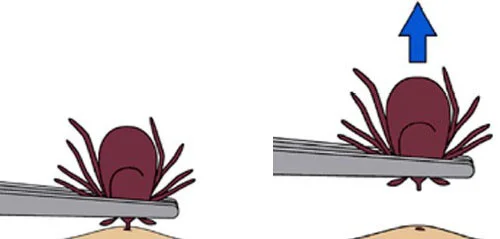
Use tweezers to effectively remove a tick attached to the body.
Typically the Ixodes tick must be attached to the skin for at least 36 hours in order to transmit Borrelia, the bacteria causing Lyme disease. This means that early detection and prompt removal of the tick will significantly reduce your chance of contracting Lyme disease. Remember to use tweezers--not your fingers or a flame--to remove the tick!
3 Stages of Disease
Lyme disease is known as the "Great imitator" because it can mimic many other diseases.
The disease is characterized by three distinct stages: early localized, early disseminated and late. Learn about the symptoms characterizing each stage of the disease.
Early Localized
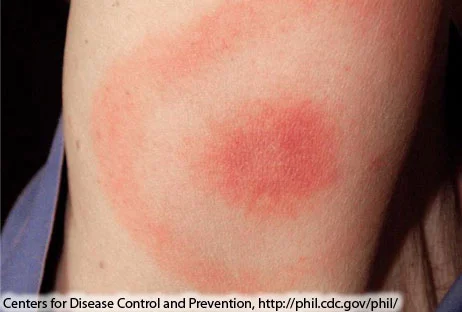
Erythema migrans is a bullseye or target like lesion that first appears at the site of the tick bite.
Erythema migrans: the classic bullseye rash associated with Lyme. About 80% of those infected with Lyme disease will develop a target-like rash at site of tick bite, usually within one month of the bite. Typically the rash isn't painful.
Non-specific infectious symptoms: feeling tired, muscle aches, joint pains, headache, neck stiffness and decrease in appetite.
Early Disseminated
Joints: joint pains that migrate from joint to joint
Nerves: neuropathy, Bell's palsy, meningitis
Skin: multiple erythema migrans on the body
Lymph nodes: inflammation and tenderness of lymph nodes
Other organ involvement: heart, eyes, liver, kidney
Late
May develop months to years after initial infection, even without previous manifestations of early localized or early disseminated phases.
Further involvement of the joints (arthritis of knee most common), nervous system and skin.
Diagnosis
Diagnosis of Lyme disease can be established by clinical history and/or laboratory testing.
Presence of erythema migrans (the classic bullseye rash) plus history of a tick bite or residing in an area with endemic Lyme disease warrants treatment. No need for confirmatory testing.
For those without the classic rash, but with suspicion for Lyme disease (e.g. tick bite, living in endemic area), blood testing can determine if you've been infected with the Borrelia bacterium.
Blood Testing
Step 1: ELISA testing for antibodies against the Borrelia bacterium. Antibodies appear in the blood 2-6 weeks following appearance of the erythema migrans rash.
Step 2: Western Blot testing. As some antibody tests can represent a false positive, Western Blot is used to confirm the diagnosis of Lyme disease.
Limitations of Blood Testing
- As antibodies take 2-6 weeks to surface in the blood, a negative result less than six weeks after the tick bite may represent a false negative.
- Antibodies typically persist years after infection, even after Lyme has been successfully treated. This makes diagnosing reinfection with Lyme much more difficult--a tricky task for those living in areas endemic to Lyme disease. The biggest clue to reinfection is the appearance of erythema migrans at a new site on the body.
Treatment
Doxycycline is the antibiotic of choice for Lyme disease.
How many milligrams, how often and for how many days? The presence of neurologic or cardiac symptoms requires more aggressive treatment.
- Absence of neurologic symptoms: 100mg Doxycycline two times per day for 10-21 days
- Presence of neurologic symptoms: 100-200mg Doxycycline two times per day for 10-28 days
- Presence of cardiac symptoms: hospitalization for administration of IV Ceftriaxone.
Unable to take Doxycycline?
If you have an allergy to doxycycline, are a pregnant or lactating woman, or are under the age of 8, consider treatment with an alternative agent: amoxicillin or cefuroxime.
Get tested and treated, if necessary:
Call: 646.568.6636
Email: Services@DoctorK.nyc
Resources
<https://www.cdc.gov/lyme/stats/maps.html>
<https://www.cdc.gov/lyme/removal/index.html>
Hu, Linden. "Clinical manifestations of Lyme disease in adults" <UpToDate.com>